Teen patient at Sidra Medicine fights back rare muscle disorder
سدرة للطب ينجح في علاج مريض مراهق مصاب بضمور عضلات
Sidra Medicine and personal determination have helped a bedridden teenager with Duchenne Muscular Dystrophy (DMD) sit up again.
DMD is a rare muscle disorder that affects approximately one in 3,500 male births worldwide. It is a genetic condition usually recognised in boys between three and six years of age.
Duchenne Muscular Dystrophy is characterised by weakness and wasting (atrophy) of the muscles of the pelvic area, followed by the involvement of the shoulder muscles.
As the disease progresses, muscle weakness and atrophy spread to additional muscles of the body, including the trunk and forearms, eventually affecting breathing capability. The disease is progressive and most affected individuals require a wheelchair by their teenage years.
Sidra Medicine, with the development of a multidisciplinary team-based approach, specialises in the care of children and young people with DMD – “providing high-quality and cutting-edge services from paediatric intensive care, surgery, therapy services to post-operative and long-term care”, according to a press statement.
Ali is a young person with DMD. Due to the rapid progression of the disease, he was wheelchair-bound by the time he was in his early teens. Despite spinal surgery at another healthcare institution in 2017, Ali’s condition continued to deteriorate. He became more immobile and was confined to his bed.
He developed severe contractures where his muscles became tight, making it painful and difficult for him to move. As a result, Ali required full support to move his body and was not able to sit up in his wheelchair.
Being bedridden and immobile for two years had a significant impact on his physical and mental health. Ali was admitted to the paediatric intensive care unit (PICU) at Sidra Medicine in mid-November of 2018.
Dr Manu Sundaram, attending physician at the PICU in Sidra Medicine, said: “Ali was admitted with a chest infection and required non-invasive ventilator support throughout the day to help him breathe. He had difficulty in tolerating feeds and was emaciated. Once he recovered from his chest infection, it became very clear that he would require full-time ventilator support for his long-term care. It was recommended that Ali undergo a tracheostomy – a necessary surgical procedure that would facilitate Ali’s breathing.”
Dr Patrick Sheehan, the division chief of Paediatric Otolaryngology, Head and Neck Surgery at Sidra Medicine, performed Ali’s tracheostomy in late-November 2018. Dr Sheehan also leads Sidra Medicine’s membership with the Global Tracheostomy Collaborative – which ensures that the tracheostomy care at Sidra Medicine is at the highest levels of practice.
Ali’s procedure involved creating an opening in his neck to place a tube into his windpipe. The tube was inserted through a cut in the neck below the vocal cords; allowing air to enter his lungs.
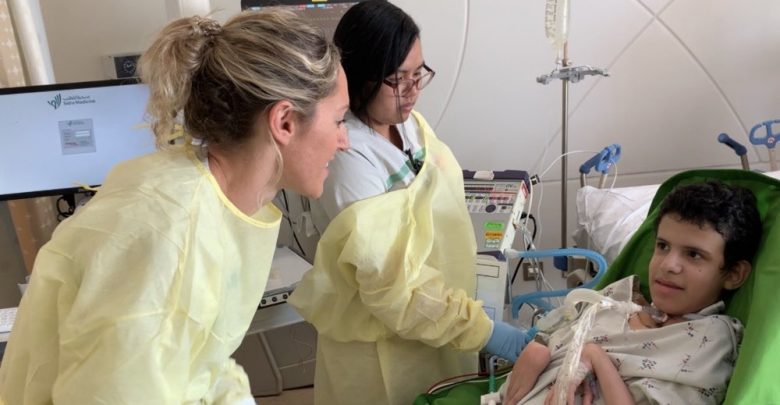
During Ali’s time at the hospital, he was taken care of by a multidisciplinary team from PICU, occupational therapy; physiotherapy; respiratory therapy; and speech and language therapy. The team, which also included dieticians and child life specialists, created a customised daily care schedule to support Ali in regaining his weight and strength; to help him with a range of movements and for him to speak with a tracheostomy.
Over four months at the Sidra Medicine PICU, with the care provided by the highly specialised multidisciplinary team, Ali slowly regained his strength and eventually was able to sit up in his wheelchair once again, the statement noted.
The transition from being horizontal for nearly two years to being able to sit up had a major impact.
“Once Ali regained his ability to sit and talk – he was keen to go out on his wheelchair and spend time in our lovely healing gardens and interact with people. It was a wonderful transformation. We are really proud of his progress and his endurance,” continued Dr Sundaram.
Kirsty Foster, one of Ali’s physical therapists, spoke of Ali’s stay and how he was not only a pleasure to work with but also made an impact on the staff working with him. “Ali has such a big personality and he was truly one of those patients who we looked forward to working with and seeing. He taught the team a lot about patience and just not giving up.”
Upon his discharge, Ali, who through speech therapy at Sidra Medicine learned to speak with the tracheostomy, managed to share a simple and powerful message with the team who helped him: “Thank you.”
تمكن مركز سدرة للطب من مساعدة مريض مراهق مصاب بمرض (حثل دوشين العضلي)، وهو اضطراب عضلي نادر يصيب مولودًا واحدًا تقريبًا من بين كل 3500 مولود ذكر حول العالم، وهي حالة وراثية تظهر لدى الأولاد الذين تتراوح أعمارهم بين ثلاثة وستة أعوام.
يتسبب المرض في ضعف وهزال ضمور عضلات منطقة الحوض، وتليها إصابة عضلات الكتف، ومع تفاقم المرض، ينتشر ضعف العضلات وضمورها إلى عضلات أخرى بالجسم، بما في ذلك الجذع والساعدين، مما يؤثر على التنفس، ويحتاج معظم الأفراد المصابين به إلى كرسي متحرك عند بلوغهم سنوات المراهقة.
ويتبنى سدرة نهجاً قائماً على الفرق متعددة التخصصات، ويتخصص في رعاية الأطفال واليافعين المصابين من خلال تقديم خدمات متطورة وعالية الجودة بدءًا من خدمات العناية المركزة للأطفال وخدمات الجراحة والعلاج وحتى رعاية ما بعد العمليات الجراحية والرعاية طويلة الأمد.
والمريض (علي) شاب صغير السن مصاب بحثل دوشين العضلي، ونتيجة للتفاقم السريع للمرض، أصبح قعيدًا على كرسي متحرك عندما بلغ أوائل سن المراهقة، وفي عام 2017، خضع لجراحة في العمود الفقري في مستشفى آخر بسبب مضاعفات، وبالرغم من الجراحة، أصبح عاجزًا عن الحركة بدرجة أكبر وكان ملازمًا الفراش.
لقد أثّرت ملازمته للفراش وعجزه عن الحركة لمدة عامين تأثيرًا بالغًا على صحته البدنية والنفسية، وقد أُدخل إلى وحدة العناية المركزة للأطفال (PICU) في سدرة للطب في منتصف نوفمبر عام 2018.
وعلى مدار أربعة أشهر في وحدة العناية المركزة للأطفال بسدرة للطب وفي ظل الرعاية التي قدمها الفريق عالي التخصص الذي يضم اختصاصات متعددة، استعاد (علي) قوته ببطء واستطاع في النهاية أن يجلس معتدلًا في كرسيه المتحرك مرة أخرى، وكان للانتقال من حالة الاستلقاء لمدة عامين تقريبًا إلى القدرة على الجلوس تأثير كبير.